By Donna Monthei, RDN, LD | EverVital Nutrition
If you’ve been wondering whether leaky gut and belly fat are connected — the answer, according to the research, is a resounding yes. And if you’ve been dieting, exercising, and still can’t budge that stubborn weight around your midsection, your gut may be working against you in ways you’d never expect.
Let me explain what’s really going on.
What Is Leaky Gut (And Why Should You Care)?
Your intestinal lining is only one cell thick, but it does an enormous job. It acts as a selective gatekeeper, allowing digested nutrients and water into your bloodstream while keeping bacteria, toxins, and undigested food particles right where they belong — inside the gut.
The cells in that lining are held together by proteins called tight junctions. Think of them as the velcro between bricks. When those tight junctions are intact, your gut barrier does its job beautifully.
But when they break down — due to a poor diet, chronic stress, gut dysbiosis, alcohol, or certain medications — gaps form between cells. Things that don’t belong in your bloodstream start sneaking through. This is what we call increased intestinal permeability, or more commonly, leaky gut.
Can Leaky Gut Cause Weight Gain? Here’s What the Research Says
Yes — and here’s the mechanism that makes it happen.
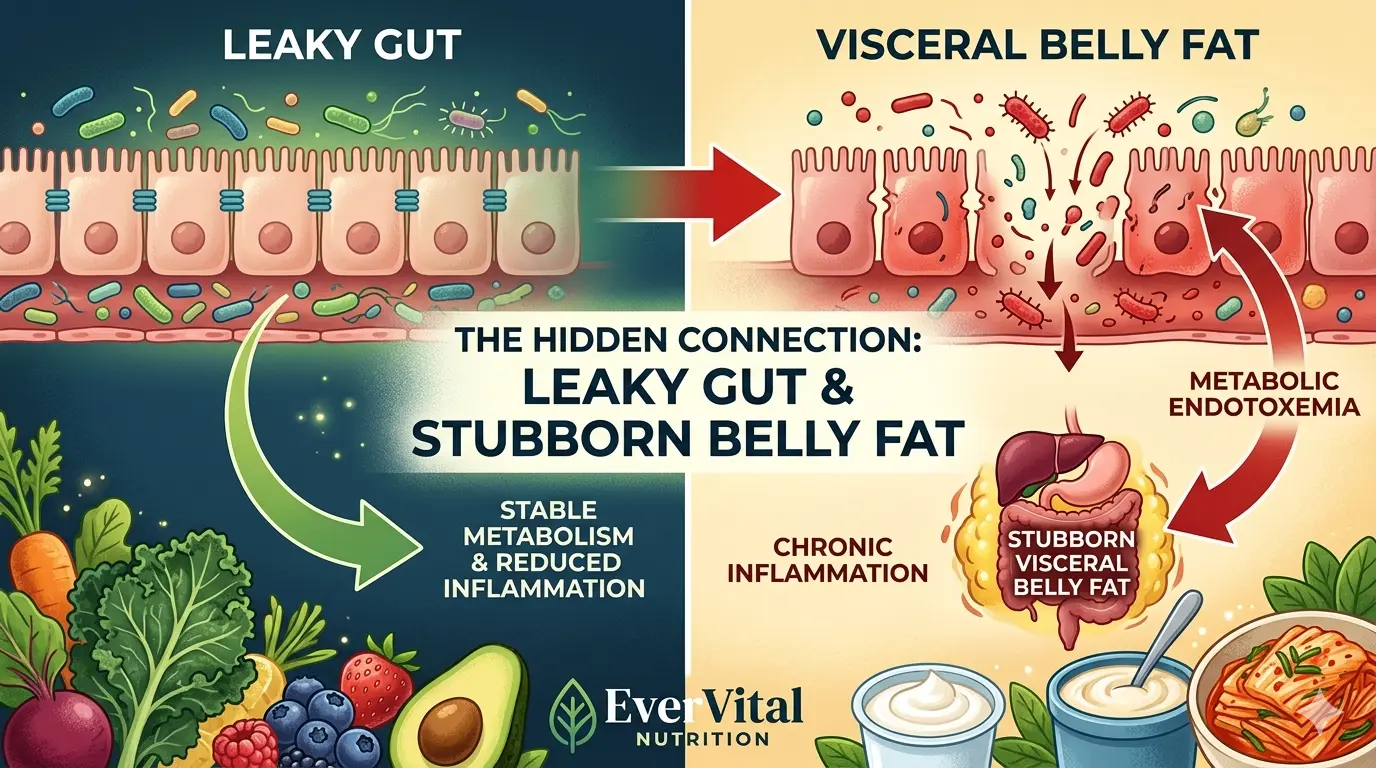
When the gut barrier is compromised, fragments from the outer walls of certain gut bacteria called lipopolysaccharides (LPS) leak into the bloodstream. In large quantities, LPS triggers your immune system to go on full alert, producing a flood of pro-inflammatory cytokines. Researchers call this state metabolic endotoxemia — a chronic, low-grade inflammatory condition that quietly drives insulin resistance, fat storage, and weight gain. (Pendaya et al, 2012).
Studies show that a high-fat diet elevates LPS levels in the bloodstream, promotes inflammation specifically in visceral adipose tissue (the deep belly fat surrounding your organs), and disrupts blood sugar regulation. When antibiotics were used in research models to reduce gut bacteria — and therefore LPS — the metabolic damage was significantly reduced. (Botany et al., 2016) That alone tells us the gut’s role in belly fat isn’t a side note. It’s central.
A landmark study published in the journal Obesity confirmed this directly. Researchers measured intestinal permeability in women using a sugar excretion test, then used CT scans and DEXA imaging to precisely measure fat distribution. The finding? Higher intestinal permeability was significantly and specifically correlated with greater visceral fat — not subcutaneous fat, not total body fat. (Gummesson et al., 2011) Just the dangerous, organ-surrounding fat that drives metabolic disease.
Leaky Gut and Belly Fat: Why It’s a Vicious Cycle
Here’s what makes leaky gut and belly fat such a frustrating combination: they fuel each other.
A high-fat, low-fiber diet damages the gut lining → LPS leaks into the bloodstream → systemic inflammation rises → insulin resistance develops → the body preferentially stores fat in the belly → that visceral fat produces its own inflammatory chemicals → gut microbiome balance is further disrupted → the gut barrier weakens even more.
Repeat.
LPS doesn’t just trigger inflammation from the outside — it actively degrades the tight junction proteins (ZO-1, aka zonulin, and occludin) that hold your gut barrier together, making permeability worse over time. (Neves et al., 2013) This is why so many people feel like they’re doing everything right and still can’t lose belly fat. They’re fighting a fire that starts in the gut, not the gym.
Calorie restriction alone will never fully break this cycle.
Visceral Fat vs. Subcutaneous Fat: Why It Matters
Not all belly fat is the same, and this distinction matters for your health.
Subcutaneous fat is the fat you can pinch on the surface — annoying, but not particularly dangerous on its own.
Visceral fat lives deep inside your abdominal cavity, wrapping around your liver, intestines, and other organs. It’s metabolically active tissue, meaning it constantly releases inflammatory signals and disrupts hormone function. Elevated visceral fat is a major driver of:
- Insulin resistance and type 2 diabetes
- Cardiovascular disease
- Non-alcoholic fatty liver disease (NAFLD)
- Hormonal imbalances
- Chronic low-grade inflammation
Two people can weigh exactly the same and have dramatically different amounts of visceral fat. That’s why waist circumference — not just the number on the scale — is such an important indicator of metabolic health.
What Causes Leaky Gut in the First Place?
Several common diet and lifestyle factors are well-established drivers of increased gut permeability:
- Ultra-processed foods and refined carbohydrates — promote dysbiosis and weaken tight junctions
- Excess fructose — especially from sugary drinks and packaged foods — has been shown to specifically degrade the proteins that hold your gut lining together
- High-fat, low-fiber diets — increase gram-negative bacteria (the LPS producers) while starving the beneficial bacteria that produce gut-protective short-chain fatty acids
- Chronic stress — sustained cortisol elevation impairs gut barrier integrity
- Alcohol — damages tight junction proteins ZO-1 and occludin with both chronic and binge-level consumption
- Gut dysbiosis — an imbalanced microbiome drives LPS overproduction and further erodes the barrier
- Low stomach acid — poor digestion upstream disrupts the entire gut environment (read more: The Role of HCl in Gut Health)
At EverVital Nutrition, we use the GI-MAP comprehensive stool test to identify exactly which bacterial imbalances, inflammatory markers, and digestive dysfunctions are contributing to a leaky gut — no guessing, no generic protocols. Just a clear picture of what’s actually happening in your gut. Learn more about our gut health testing and programs here.
How to Heal Leaky Gut and Reduce Belly Fat
If visceral fat is driven in part by gut permeability and chronic metabolic endotoxemia, then healing the gut becomes a powerful strategy for addressing belly fat — not by eating less, but by eliminating the underlying inflammation driving fat storage in the first place.
Here’s where to start:
1. Feed Your Gut Bacteria — Fiercely
Fiber is the single most important dietary factor for gut barrier health. Diverse plant foods fuel the bacteria that produce butyrate — a short-chain fatty acid that literally powers the cells lining your gut (colonocytes) and strengthens tight junctions from the inside. No fiber → no butyrate → weak gut lining → leaky gut. Aim for 30+ grams of fiber daily from a wide variety of vegetables, fruits, legumes, and whole grains. Read more: The Power of Butyrate for Gut Health
2. Eat Fermented Foods Every Day
Kimchi, sauerkraut, kefir, and plain yogurt with live cultures introduce beneficial bacteria and support a diverse microbiome. Microbial diversity is one of the strongest predictors of gut barrier health and metabolic resilience.
3. Eliminate Ultra-Processed Foods
Processed foods drive dysbiosis, increase gram-negative bacteria (LPS producers), and deliver excess fructose and refined fats that specifically degrade tight junctions. Every whole-food swap matters — and the results compound over time.
4. Prioritize Adequate Protein
Protein supports gut repair, preserves the muscle mass that keeps your metabolism running, and has a higher thermic effect than carbs or fat — meaning your body burns more calories just digesting it. Distributing protein across meals (rather than loading it at dinner) improves muscle protein synthesis and metabolic outcomes. Read more: Optimal Protein for Gut Health
5. Manage Stress Like a Health Intervention
Chronic stress raises cortisol, which promotes gut permeability and directly signals the body to store fat viscerally. Sleep hygiene, stress reduction practices, and nervous system regulation aren’t optional extras — they’re core gut healing interventions.
6. Get Targeted Gut Testing
General advice only gets you so far. Specific imbalances — an overgrowth of gram-negative bacteria, low beneficial bacteria, high inflammatory markers, compromised secretory IgA — require targeted, personalized protocols. This is exactly what the GI-MAP test makes possible. Schedule your complimentary gut assessment to find out what’s driving your symptoms.
Frequently Asked Questions About Leaky Gut and Belly Fat
Can leaky gut cause belly fat? Yes. Research shows that increased intestinal permeability allows bacterial endotoxins (LPS) to enter the bloodstream, triggering metabolic endotoxemia — a state of chronic low-grade inflammation that drives insulin resistance and preferential fat storage in the visceral (belly) region. A landmark study found a direct correlation between gut permeability and visceral fat area, independent of total body fat.
How do I know if leaky gut is causing my weight gain? Common signs that leaky gut may be contributing to your weight struggles include: stubborn belly fat that doesn’t respond to diet and exercise, bloating and digestive discomfort, food sensitivities, brain fog, skin issues, and chronic fatigue. The most accurate way to assess gut barrier function and microbiome health is through comprehensive stool testing like the GI-MAP. Take our free Gut Health Quiz to get a personalized starting point.
Does healing leaky gut help with weight loss? Addressing gut barrier dysfunction can support healthier metabolic function, reduce chronic inflammation, improve insulin sensitivity, and create an internal environment more conducive to fat loss — especially visceral fat reduction. It’s not a magic bullet, but for many people with weight loss resistance, gut health is the missing piece.
What foods heal a leaky gut? Focus on high-fiber plant foods (vegetables, fruits, legumes, whole grains), fermented foods (kimchi, kefir, sauerkraut, yogurt), adequate quality protein, and anti-inflammatory fats like olive oil and fatty fish. Minimize ultra-processed foods, excess sugar, alcohol, and refined seed oils, which are known to damage the gut barrier.
How long does it take to heal leaky gut? It varies significantly based on the severity of the dysbiosis and damage, your diet, stress levels, and other individual factors. With a targeted, personalized protocol, many people begin to notice improvements in digestive symptoms within 4–8 weeks. More significant restoration of gut barrier integrity and metabolic markers typically takes 3–6 months of consistent effort.
The Bottom Line
If you’ve been frustrated by belly fat that won’t budge no matter what you do — your gut may be telling you something important.
The science is clear: a compromised gut barrier drives the kind of chronic inflammation that fuels visceral fat accumulation, insulin resistance, and metabolic dysfunction. Addressing leaky gut isn’t a trendy wellness hack — it’s a metabolically sound strategy backed by peer-reviewed research.
The good news? The gut responds remarkably well to the right interventions. Not by starving yourself. Not by running yourself into the ground. But by rebuilding the foundation of your metabolic health from the inside out — with a clear picture of what’s actually happening in your gut, and a personalized plan designed around you.
At EverVital Nutrition, that’s exactly what we do.
👉 Schedule your complimentary gut assessment or take our free Gut Health Quiz to get started today.
Donna Monthei is a Registered Dietitian and gut health nutritionist at EverVital Nutrition, specializing in GI-MAP comprehensive testing and personalized gut healing protocols for people struggling with chronic digestive issues, weight loss resistance, and metabolic dysfunction.
References
Boutagy, N. E., McMillan, R. P., Frisard, M. I., & Hulver, M. W. (2016). Metabolic endotoxemia with obesity: Is it real and is it relevant? Biochimie, 124, 11–20. https://doi.org/10.1016/j.biochi.2015.06.020
Gummesson, A., Carlsson, L. M. S., Storlien, L. H., Bäckhed, F., Lundin, P., Löfgren, L., Stenlöf, K., Lam, Y. Y., Fagerberg, B., & Carlsson, B. (2011). Intestinal Permeability Is Associated With Visceral Adiposity in Healthy Women. Obesity, 19(11), 2280–2282. https://doi.org/10.1038/oby.2011.251
Neves, A. L., Coelho, J., Couto, L., Leite-Moreira, A., & Roncon-Albuquerque, R. (2013). Metabolic endotoxemia: a molecular link between obesity and cardiovascular risk. Journal of Molecular Endocrinology, 51(2), R51–R64. https://doi.org/10.1530/jme-13-0079
Pendyala, S., Walker, J. M., & Holt, P. R. (2012). A High-Fat Diet Is Associated With Endotoxemia That Originates From the Gut. Gastroenterology, 142(5), 1100–1101.e2. https://doi.org/10.1053/j.gastro.2012.01.034